With excoriation disorder (aka skin picking, or, dermatillomania) only being recognized as an independent mental health disorder in 2013, misdiagnoses of this compulsion is still common. From dermatological issues to other mental health afflictions, excoriation disorder can be misdiagnosed as several conditions before being properly addressed and treated.
Misdiagnoses
Acne
Many people pick at their acne, and it can be difficult to distinguish if it is the trigger or separate from a compulsive disorder. Although one DSM-5 criteria for excoriation disorder dictates “The symptoms are not caused by a substance or medical, or dermatological condition”, the behavior can still be present after dermatological concerns are addressed.
Atopic Dermatitis
Also known as eczema, atopic dermatitis is an auto-immune condition that presents itself with rashes on itchy or dry skin. With flare-ups of scratched skin being common with ezcema, dermatologists or general practitioners do not have training to diagnose excoriation disorder and may prescribe topical creams instead of recognizing mental health as the root cause.

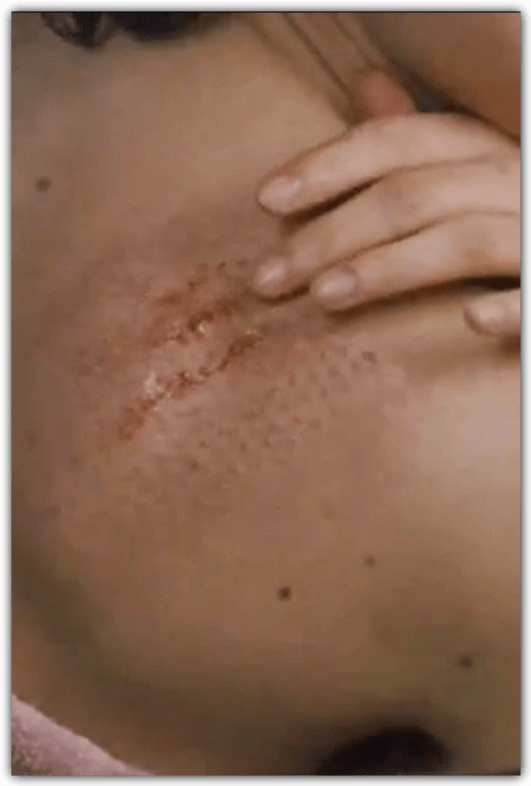
Delusional Parasitosis or Morgellons?
Delusional Parasitosis
A rare psychiatric disorder in which a person believes they have parasites under their skin, resulting in attempts to remove them. Also known as Ekbom’s syndrome, it is usually accompanied by sensory hallucinations of a crawling feeling on or under the skin, and is diagnosed when no other delusions are present and symptoms have persisted for over a month.
Lichen Simplex Chronicus
Presenting itself as a thickening of skin, lichen simplex chronicus is a dermatological condition caused by repetitive scratching of patchy, dry, areas. Also known as neurodermatitis, this misdiagnosis can easily come from the belief that the manifestation of itchiness is the cause of the scratching.
Morgellons Disease
A controversial condition, Morgellons disease is considered to be a sub-type of delusional parasitosis that involves a person consistently removing fibers from their skin. Fascinating in its epidemiology, many professionals claim that the material extracted from patients is from their clothing or environment- not an internal source, as often self-reported.
Although the behavior of someone with Morgellons is similar to excoriation disorder, the intention of the act differs greatly. Compulsive skin pickers are trying to fix a real or perceived/ exaggerated imperfection on the skin or repetitively self-soothe, while those with Morgellons search for fibers to get rid of.
Considered to be a delusional infestation, Morgellons disease is often treated with anti-psychotic medication to reduce or eliminate the pervasiveness of this serious condition.

about Morgellons Disease
Obsessive-Compulsive Disorder (OCD)
While skin may be the considered to be the obsession, and picking the compulsion, excoriation disorder is not the same as OCD. Body-Focused Repetitive Behaviors (BFRBs) may relate to OCD with one being driven to repetitively engage in the behavior, but BFRBs provide a sensory relief whereas completing an OCD task or ritual only quells the panic, often providing no relief.
To better categorize obsessions and compulsions, the DSM-5 includes a new Obsessive-Compulsive and Related Disorders section, where excoriation disorder is found.
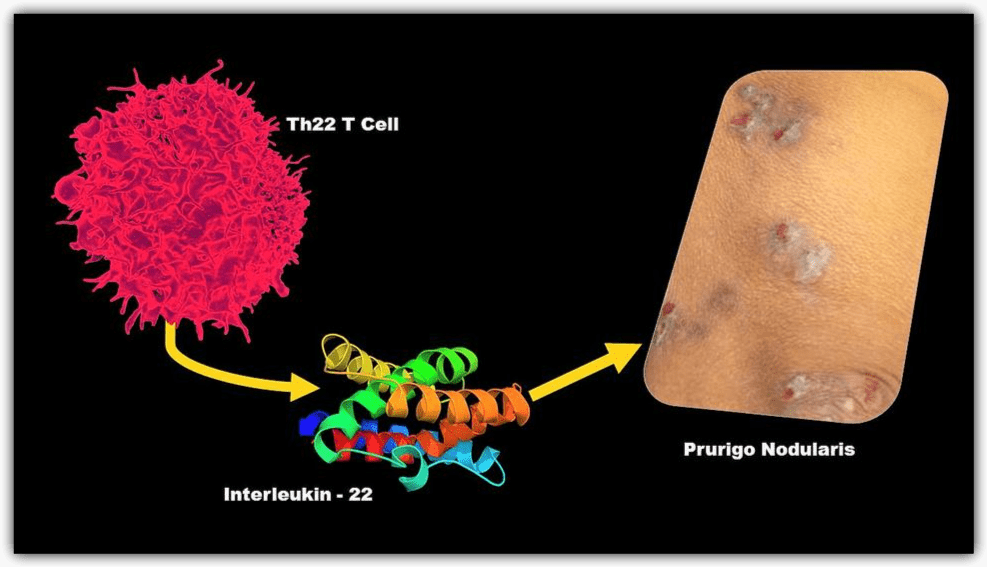
Prurigo Nodularis
A chronic skin condition that presents with hard and itchy bumps, prurigo nodularis may be misdiagnosed by a professional if the skin picker notes itchiness as a cause for engaging in the behavior.
The bumps, known as nodules, are often the result of repetitive scratching.
Self-Harm
With dermatillomania resulting in damage to the skin, many people believe that it is another form of self-harm, similar to cutting or burning oneself. While all are physical acts done to oneself to cope with emotional distress or sensory imbalances, the urge to engage in excoriation is overwhelming due to its compulsive nature.
The most significant difference between skin picking and self-harm is intention. Excoriation disorder manifests as a compulsion while self-harming behaviors often presents as deliberate actions to inflict pain, or see blood, among other reasons. Also known as entering a trance-like state, skin pickers can become so focused on removing an imperfection that they block out accompanying pain, intent on “fixing” the irregularity.
Trichotillomania
A sister-syndrome to excoriation disorder and another Body-Focused Repetitive Behavior (BFRB), trichotillomania is defined by the compulsive need a person has to pull out hair on their hair, face, or body. Diagnosable in previous versions of the DSM, trichotillomania is now an outdated diagnosis for skin pickers because of the inclusion of excoriation disorder in 2013.
With both conditions sharing many traits, they are treated with similar methods, particularly Cognitive Behavioral Therapy (CBT) and mindfulness strategies to reduce urges and manage triggers.

trichotillomania (or TTM)
Misconceptions
A “Bad Habit”
While those with a milder form of dermatillomania may relate to having a bad habit, this terminology diminishes the seriousness and severity of what excoriation disorder entails.
Addiction
Although a simple blood test can determine if a person’s skin picking is caused by using drugs (methamphetamine, heroin, etc), people who compulsively pick their skin can be mistaken for addicts, which creates more stigma and can lead to discrimination that results in poor healthcare treatment, or being dismissed with any health concern.
AIDS/ HIV
With various skin conditions leading to rashes and sores in those who have AIDS or HIV, an assumption that can be made about skin pickers is that their marks are from Kaposi’s sarcoma, a type of skin cancer that can occur in the later stages of HIV when the T4 cell count is low. The stigma and misinformation often associated with AIDS can lead to skin pickers being mistreated in a clinical setting.
Monkeypox*
After experiencing over two years of collective fear and trauma caused by the pandemic, the anxiety of contracting a sickness has been transferred from COVID-19 to monkeypox. With countries around the world declaring monkeypox a public health emergency in 2022, the stigma in having skin conditions has increased with many reporting unsolicited comments or harassment related to this infectious disease.
Monkeypox is known to present as a pus-filled bump, blistery, or open sore. It goes through many stages of healing, creating scabs that may look like excoriation disorder with those infected reporting between 10 and 150 spots on their skin.
* If you have excoriation disorder and suspect you may have monkeypox, keep spots covered to avoid picking them and contact your primary care physician to learn about treatment protocols in your area.
If you are seeking a diagnosis from a professional, a dermatologist can rule out possible skin conditions. Psychologists, psychotherapists, and psychiatrists are qualified to determine if your skin picking is caused by excoriation disorder or if it is better explained as a symptom of another mental health condition.